
Introduction
Topical product formulation development is the structured, science-led process of designing and optimizing a product applied to the skin — cream, serum, gel, or lotion — by selecting and combining ingredients to achieve a defined performance, safety, and stability profile.
For personal care brands, in-house R&D teams, and product developers, getting this process right determines whether a product performs as claimed, clears regulatory review, and scales without failures.
The numbers reflect the stakes: 76.8% of FDA cosmetic recalls stem from microbial contamination02898-6/fulltext), making robust formulation development critical to brand protection. Every ingredient choice, stability test, and scale-up decision shapes whether your product reaches consumers safely and performs as claimed.
This guide covers how topical formulation development works from start to finish, what ingredients and variables drive outcomes, and where most teams lose time — from brief definition and prototype development through stability testing and commercial manufacturing.
TL;DR
- Topical formulation development transforms a product concept into a safe, stable, scalable finished good through structured stages
- The process includes concept definition, prototype formulation, stability and safety testing, and scale-up validation
- Vehicle type (cream, gel, serum, ointment) determines active delivery, texture, and long-term stability
- Critical variables include ingredient compatibility, pH control, emulsification chemistry, preservative efficacy, and process parameters
- Early-stage errors in emulsifier selection or skipped stability studies cause failed scale-ups and costly reformulations
What Is Topical Product Formulation Development?
Topical product formulation development is the iterative, science-based process of identifying the right combination of active and functional ingredients, vehicle systems, and processing conditions to create a topical product that performs consistently, safely, and at scale.
A finished formulation must meet four core requirements:
- Delivers its claimed benefit — moisture, UV protection, anti-aging, or cleansing
- Remains stable under real-world storage conditions
- Feels acceptable to the consumer (texture, skin feel, spreadability)
- Meets regulatory safety thresholds for its intended market
Under EU Regulation 1223/2009, a cosmetic product is defined as "any substance or mixture intended to be placed in contact with the external parts of the human body with a view exclusively or mainly to cleaning them, perfuming them, changing their appearance, protecting them, keeping them in good condition or correcting body odours."
Formulation development is distinct from ingredient sourcing or contract manufacturing — it precedes both and defines the blueprint that enables scale-up. Skipping this step typically surfaces later as stability failures, reformulation costs, or regulatory rejections — problems far more expensive to fix post-launch.
How the Topical Formulation Development Process Works
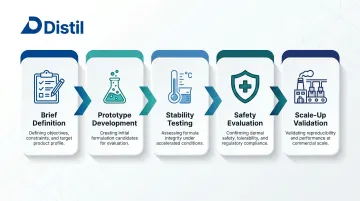
Formulation development moves through five interconnected stages, each building on the output of the previous:
Step 1: Brief Definition and Concept Alignment
Formulation begins not in the lab, but with a structured product brief that captures:
- Target skin type and intended benefit
- Desired texture, finish, and sensory profile
- Actives of interest and performance expectations
- Regulatory market requirements (India, EU, US)
- Cost-of-goods targets and margin constraints
Poor brief definition is the leading cause of reformulation cycles. A vague brief without clarity on target market or texture leads to prototypes that fail consumer testing or regulatory review.
Step 2: Prototype Development and Ingredient Selection
Formulators design an initial prototype by selecting a vehicle system — emulsion (oil-in-water or water-in-oil), gel, anhydrous, or micellar — matched to the product's delivery goals. Then functional ingredients are layered in:
- Emulsifiers to stabilize oil and water phases
- Humectants like hyaluronic acid and glycerin to draw moisture
- Emollients such as coco-caprylate/caprate and octyldodecanol for smooth spreadability
- Actives (UV filters, peptides, botanical extracts)
- Thickeners to control viscosity and texture
- Preservatives to prevent microbial growth
Each ingredient must be evaluated for compatibility with others and with the chosen base. For example, using zinc oxide UV filters in a water-based gel requires pre-dispersed systems to prevent agglomeration and maintain SPF performance.
Step 3: Stability Testing
Prototypes undergo accelerated and real-time stability testing to detect phase separation, viscosity changes, color shifts, active degradation, and microbial contamination.
ICH Q1A(R2) specifies accelerated conditions of 40°C ± 2°C / 75% RH ± 5% RH for 6 months. The cosmetics industry commonly adapts this to 45°C for 3 months, which predicts approximately 2 years at room temperature.
Standard monitoring parameters include:
- Organoleptic: color, odor, fragrance
- Physical: viscosity, pH, texture, flow
- Microscopic: particle size uniformity
- Integrity: emulsion separation, creaming
- Microbiological: bacterial, mold, yeast counts

Skipping or shortcutting stability testing is a common and costly error. Brands attempting to launch with only 4–6 weeks of accelerated data miss slow-onset degradation such as preservative depletion or fragrance drift.
Step 4: Safety and Performance Evaluation
Dermal safety assessment confirms the formulation is safe for intended use. This includes:
- Patch testing (HRIPT conducted over 6 weeks with 50–200 subjects)
- In-use performance testing to validate efficacy claims
- Sensory evaluation for texture, spread, absorption, and skin feel
ISO 11930 preservative efficacy testing is required for water-containing products, using test organisms including E. coli, S. aureus, P. aeruginosa, C. albicans, and A. brasiliensis over 28 days at 32.5°C. Regulatory authorities in the EU, US, and India increasingly require documented substantiation before claims can be made — so testing records and study reports need to be archived alongside the formula itself.
Step 5: Scale-Up and Manufacturing Alignment
Translating a lab-bench formula to commercial batch production requires adjusting process parameters — mixing speed, temperature profiles, phase addition sequence, batch size geometry.
Key process variables that change at scale:
- Heat transfer: A batch cooled in 20 minutes (bench) versus 120 minutes (production) produces different microstructures affecting viscosity
- Shear rate: High-speed mixing can introduce aeration, changing specific gravity
- Reynolds Number: Turbulence onset at NRe > 2,000 affects emulsion droplet size
- Power consumption: Proportional to impeller speed cubed and diameter to the fifth power
Without deliberate process documentation, these variables cause microstructure and performance to shift between bench and production — sometimes subtly enough to pass initial QC but fail in field. Managing that complexity requires formulators who stay involved through scale-up, not just through lab sign-off. Teams with backgrounds spanning both R&D and manufacturing — such as Distil's, which includes experience from L'Oréal and BASF — handle trials, process documentation, and manufacturing alignment as a single continuous workstream rather than sequential handoffs.
Key Ingredients and Their Role in Topical Formulations
Vehicle or Base System
The carrier — water-in-oil emulsion, oil-in-water emulsion, gel, anhydrous balm — defines texture, occlusion level, and how actives are delivered to the skin.
Vehicle comparison:
| Vehicle Type | Composition | Key Characteristics | Typical Applications |
|---|---|---|---|
| Ointment | <20% water; >50% hydrocarbons/waxes | Highly occlusive; increases active penetration | Thickened/lichenified skin |
| Cream | Emulsion (W/O or O/W); 15–40% oil, 45–80% water | More spreadable than ointment | Weepy/exudative skin |
| Lotion | >50% water; 10–15% oil, 75–85% water | Lightest semisolid; easiest to apply over large areas | Body lotions |
| Gel | Liquefies on skin contact; provides cooling | Best for hairy areas (scalp), oily skin | Face gels, hair products |
| Serum | Lightweight; water or silicone-based; high active concentration | Targeted delivery of actives | Anti-aging, brightening |

Emulsifiers and Stabilizers
In emulsion-based products (creams, lotions), the emulsifier system determines droplet size, phase stability, and shelf life.
HLB (Hydrophilic-Lipophilic Balance) values guide emulsifier selection:
- HLB < 8 (ideal 4–5): Water-in-oil emulsions
- HLB 8–15: Oil-in-water emulsions
- HLB > 15: Solubilization
HLB balance, concentration, and combination of primary and co-emulsifiers must be tuned to the oil phase composition and desired rheology.
Functional Actives
Actives deliver the claimed benefits:
- Humectants (glycerin, hyaluronic acid) draw moisture into skin (effective when atmospheric humidity >80%)
- Occlusives (petrolatum reduces TEWL by >98%; mineral oil and lanolin by 20–30%) create barriers to prevent transepidermal water loss
- Emollients (neopentyl glycol diheptanoate, trimethylolpropane tricaprylate/tricaprate) soften and smooth skin
- UV filters (zinc oxide, titanium dioxide) protect against UV damage
- Peptides and botanical extracts deliver anti-aging and skin-conditioning benefits
Concentration, solubility in the chosen vehicle, and interaction with other ingredients determine whether efficacy claims can be substantiated. Getting the active ingredient selection right is only part of the equation — keeping the formulation stable and safe over its shelf life introduces an equally demanding set of decisions.
Preservatives and the Challenge of Preservation
Multi-phase and water-containing formulations require effective antimicrobial preservation to pass challenge testing. Preservative choice is constrained by:
- Regulatory status in each target market (EU Annex V, FDA GRAS, India Cosmetics Rules)
- pH sensitivity and compatibility with other ingredients
- Consumer demand for low-irritation systems
The global clean beauty market — valued at $10.49 billion (2025) and projected to reach $35.30 billion by 2033 (CAGR 16.8%) — drives demand for preservative-free formulations. "Preservative-free" claims require alternative strategies such as:
- Low water activity (below 0.60–0.70)
- Anhydrous systems
- pH adjustment
- Multifunctional antimicrobial ingredients
- Airless packaging
All self-preserving formulations must still pass ISO 11930 challenge testing.
Rheology Modifiers and Thickeners
Polymers and gelling agents (carbomers, cellulose derivatives, xanthan gum) control viscosity, spreadability, and sensory profile. Selection must account for:
- Compatibility with ionic ingredients
- pH range stability
- Manufacturing shear conditions
A thickener that performs at lab scale may behave differently under high-shear commercial mixing — viscosity can shift from 85,000 cP to 140,000 cP based on process changes alone.
Common Formulation Mistakes and When to Rethink Your Approach
Most Costly Early-Stage Error: Marketing-Driven Ingredient Selection
Selecting ingredients based on marketing appeal or supplier availability rather than formulation function — such as adding a trendy active without verifying its solubility, stability at required pH, or compatibility with preservatives — forces full reformulation after stability failure.
Incorporating a peptide into a low-pH vitamin C serum without confirming peptide stability at pH 3.0, for instance, results in active degradation within weeks.
The Misconception That Stability Testing Can Be Shortened
Many brands attempt to launch after only 4–6 weeks of accelerated stability data. This is insufficient for detecting:
- Long-term phase instability
- Active degradation below label claim
- Preservative depletion
- Fragrance drift
Minimum testing timelines for responsible commercialization:
- Accelerated stability: 3 months at 45°C
- Real-time stability: 12 months at 25°C
- Freeze-thaw cycling: Minimum 3 cycles of -10°C to 25°C
Reformulation costs range from $50,000 to $200,000 per product, with product launches frequently delayed while scale-up issues are resolved.
The Scale-Up Assumption Problem
Teams often assume a formula that works in a 200g lab batch will behave identically at 500kg. Key process variables that change at scale include:
- Heat transfer efficiency
- Shear rate and mixing intensity
- Emulsification droplet size distribution
- Batch geometry and vessel configuration
This assumption leads to off-spec batches, sensory complaints, or stability failures in the first commercial run.
Bridging that gap requires unified oversight across R&D and manufacturing. Distil's formulation team — drawing on backgrounds from BASF and L'Oréal — manages trial batch oversight, process documentation, and quality systems from prototype through commercial production, keeping lab intent and manufacturing output aligned.
When to Redirect the Formulation Approach
If a formula consistently fails stability under specific conditions, if cost-of-goods at commercial scale exceeds target margin, or if a key ingredient faces regulatory restriction in the target market, the correct response is structured reformulation with revised constraints — not incremental tweaks.
Signals that a formula requires strategic reformulation:
- Repeated preservative failures
- Emulsion instability at temperature extremes
- Active degradation below label claim within stability window
- Microbial contamination in finished batches

Iterating without strategic direction burns both time and budget. A reformulation brief that locks in regulatory limits, cost-of-goods targets, and performance benchmarks upfront gives the team a defined decision framework — and shortens the path to a stable, commercial-ready formula.
Conclusion
Topical product formulation development is a structured, multi-stage technical process that transforms a product concept into a safe, stable, scalable finished good. The pipeline demands scientific rigor at every stage — from brief definition through prototype development, stability testing, safety assessment, and scale-up validation.
Brands that invest in proper formulation development reduce reformulation costs, protect their product IP, and reach market faster. Those that skip stages or rely on unevaluated bases risk consumer safety, regulatory rejection, and failed scale-ups.
Across a complete development cycle, that means:
- Defining performance and regulatory targets before formulation begins
- Validating stability and safety before any commercial commitment
- Confirming scale-up at pilot stage to avoid late-stage failures
For brands seeking integrated formulation development — from ingredient selection through commercial-scale manufacturing — Distil partners with brands across the full development pipeline: R&D-led formulation, application-specific trials, unified quality oversight, and scale-up through a network of 20+ vetted manufacturing partners in India.
Frequently Asked Questions
What is the difference between a cream, gel, serum, and ointment formulation?
The key difference is the vehicle system. Creams are water-oil emulsions; gels are gelling-agent-based in water or alcohol; serums are lightweight, high-active water systems; ointments are anhydrous occlusive bases. Each choice directly affects texture, skin feel, and how actives are delivered.
How long does topical product formulation development typically take?
Timeline varies by product complexity, but typically ranges from 3 to 12 months from concept to validated, scale-ready formulation. Accelerated stability studies take a minimum of 3 months, and safety and performance testing add further time depending on the target market's requirements.
What stability tests are required for a topical personal care product?
Standard stability testing covers accelerated (elevated temperature and humidity), freeze-thaw cycling, and real-time ambient storage. Key parameters include pH, viscosity, colour, odour, phase separation, active assay, and microbial challenge — with exact requirements varying by target market.
Why do formulations that work in the lab fail at commercial scale?
Lab-to-scale failures typically result from differences in shear rate, batch geometry, temperature control, and mixing time — variables that affect emulsification, microstructure, and active distribution. Proper process documentation and scale-up trials are required to bridge this gap.
What is preservative efficacy testing and why is it required?
Preservative efficacy testing (PET) verifies that a product's preservation system prevents microbial growth under real-world use and storage conditions. It is a regulatory requirement in most markets for water-containing leave-on and rinse-off products.
When should a brand consider reformulating an existing product?
Reformulation is warranted when a key ingredient is restricted or banned in a target market, when stability data reveals performance decline below specification, when consumer complaints indicate sensory or efficacy issues, or when cost-of-goods must be optimised for commercial viability.



